We invite you to enhance and rejuvenate your natural beauty in an atmosphere of serenity and advanced aesthetic technology.

Plastic Surgery
With over twenty-five years of cosmetic plastic surgery experience, Dr. Gwen Maxwell is Board Certified by the American Board of Plastic Surgery and well known for the beautiful and natural looking results she achieves for her patients.

Med Spa
The Med Spa enhances both physical beauty and inner well being, offering a full spectrum of both skin and body care services. It is our goal to provide you with a highly skilled staff and state-of-the-art equipment.
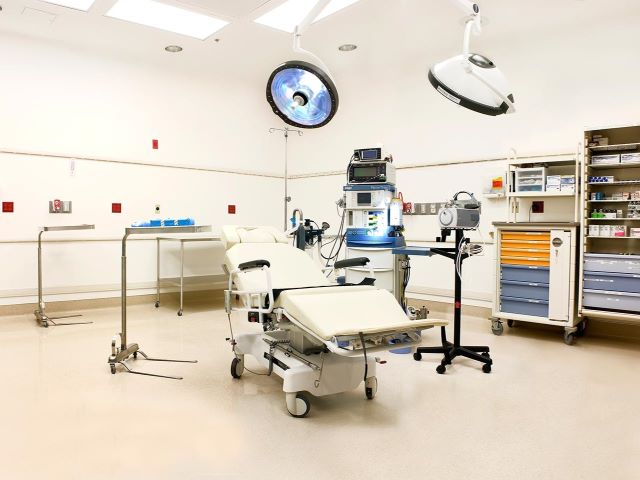
Surgery Centers
Most surgical procedures are performed at surgery centers certified by the AAAASF, the State of Arizona, and Medicare.
Sign-up today to receive limited time offers and specials.